Postpartum belly fat can feel frustrating, confusing, and far more stubborn than anyone prepared you for. You delivered a baby, came home exhausted and completely in love, and somewhere between the diaper changes and the 3 a.m. feedings, you stood in front of the mirror and wondered: why does my belly still look like this?
Nobody warned you about that part. The books covered labor and breastfeeding. Nobody sat you down and said your belly would take a real while, or explained why.
Quick Answer: Postpartum belly fat is driven by uterine recovery, hormonal changes, diastasis recti, sleep deprivation, and elevated cortisol. Most women see significant improvement between 6 and 12 months with consistent walking, strength training, adequate protein, and realistic expectations. There are no shortcuts, but there is a clear path forward.
This article gives you the honest, science-backed answer. No toxic positivity, no unrealistic timelines. Your postpartum belly is not failing you. It is healing. And understanding what is actually happening inside your body is the first step toward doing something meaningful about it.

Quick Postpartum Belly Fat Recovery Plan
If you want the condensed version first, here it is. This plan is what the evidence actually supports. No fluff, no miracle claims.
Daily habits that move the needle:
- Walk every day. Start with 10-15 minutes. Build toward 30-45 minutes by week 6. This is your most important early tool.
- Hit 25-30g of protein per meal. Eggs, Greek yogurt, chicken, cottage cheese, lentils. Protein preserves muscle and controls hunger.
- Drink enough water. At least 8-10 cups daily. Nursing mothers need 13+ cups. Dehydration mimics hunger.
- Protect your sleep. You cannot control a newborn’s schedule, but you can go to bed when they do. Sleep deprivation physically blocks fat loss.
- Do not crash diet. Breastfeeding mothers need at least 1,800 calories. Severe restriction raises cortisol and stalls progress.
After your 6-week clearance:
- Add 2-3 strength training sessions per week (bodyweight is enough to start).
- Begin core rehabilitation: breathing, pelvic floor work, and gentle deep core exercises before any crunches or sit-ups.
- Check for diastasis recti before doing any traditional ab exercises.
Timeline reality check:
- Weeks 1-6: Focus on healing, not fat loss.
- Months 2-6: Consistent effort produces visible change.
- Months 6-12: Most significant postpartum belly improvement happens here.
Stick with this for 6 to 12 months. That is the actual timeline, and it is completely normal.
Why Postpartum Belly Fat Is Different
Most fitness content gets this completely wrong. Your postpartum belly is not the result of overeating or inactivity. It has multiple overlapping biological causes, and treating it like ordinary weight gain is exactly why so many women feel like they are doing everything right and still not seeing results.
Here is what is actually going on:
- Your abdominal muscles separated during pregnancy to accommodate your baby.
- Your uterus expanded to roughly 500 times its normal size.
- Your hormones shifted dramatically within hours of delivery.
- Your sleep became severely fragmented.
- Your body, responding to all of this, is doing exactly what biology designed it to do: protect you during recovery.
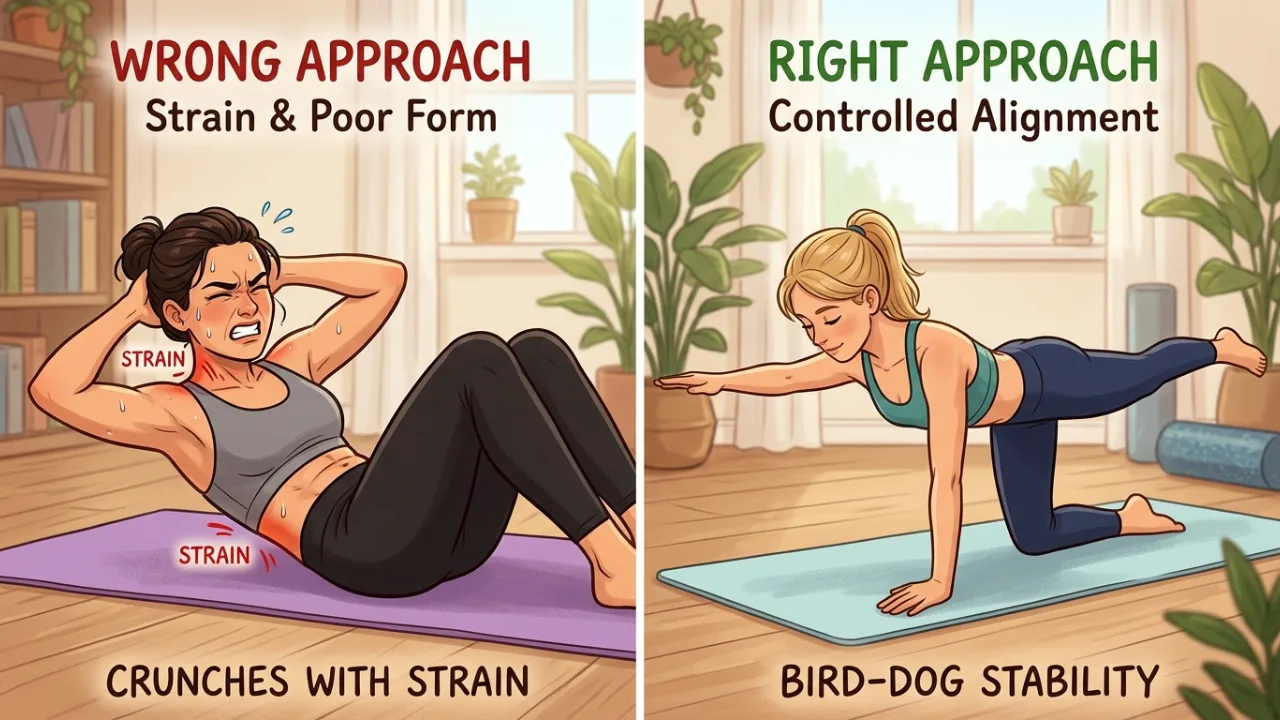
The wrong approach (jumping into crunches, slashing calories) can make things measurably worse. The right approach, timed correctly and done consistently, works.

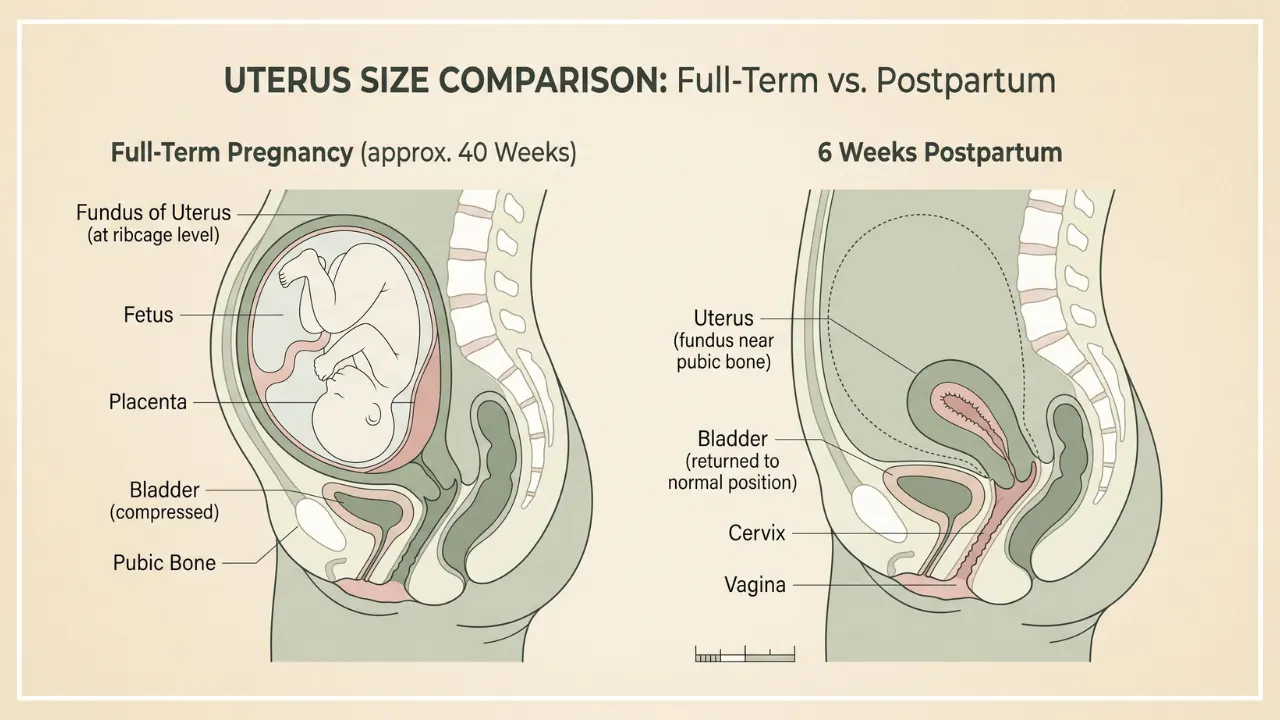
Your Uterus Is Still Shrinking
In the early weeks after delivery, a significant portion of what looks like belly fat is simply your uterus returning to its pre-pregnancy size. During pregnancy, your uterus weighs roughly 1,000 grams. After delivery, it gradually contracts back down to 50-100 grams through a process called involution, which takes approximately six to eight weeks.
What this means practically: If you are two weeks postpartum and still look visibly pregnant, a substantial part of that is a healing organ, not fat. Give your body time before drawing conclusions about progress.
Breastfeeding releases oxytocin, which accelerates uterine contractions and speeds up involution slightly.This is one of the clearer physical recovery benefits of nursing in the early weeks.
Hormones, Breastfeeding, and Fat Storage
The hormonal shift after delivery is dramatic and widely underestimated. Estrogen and progesterone plummet within hours of delivering the placenta. This triggers milk production, mood changes, and in many women, water retention that looks like fat.
If you are breastfeeding, elevated prolactin continues to suppress estrogen. This signals your body to maintain fat reserves around the abdomen and hips as a biological buffer for lactation.
A comparative study found that nursing mothers show different abdominal fat distribution patterns than formula-feeding mothers, with slower belly fat loss in the early months, though total weight loss over twelve months tends to equalize.
Breastfeeding burns 300-500 extra calories daily, which sounds like it should help. But nursing hormones can simultaneously signal fat preservation, especially around the lower belly. Many women find the postpartum belly pooch barely shifts while nursing, then changes rapidly after weaning. Others lose weight steadily throughout. Both are biologically normal.
The takeaway: Breastfeeding is not a reliable fat loss strategy on its own, and you should not stop nursing for weight loss reasons. If progress is slow while nursing, your body is likely doing exactly what it is supposed to.
One hard limit: According to the Academy of Nutrition and Dietetics, nursing mothers should consume at least 1,800 calories per day during lactation. Going below this level can impact the quality and quantity of breast milk and compromise infant growth.
Cortisol, your stress hormone, is also elevated postpartum for most women, driven by sleep deprivation, emotional load, and the demands of newborn care. Chronically elevated cortisol specifically drives abdominal fat storage, a mechanism well-documented in the endocrinology literature.This is why stress management is a metabolic issue, not just a wellness suggestion.
The hormonal environment typically becomes more favorable for fat loss after weaning or around the six-month mark. Knowing this can help you stop blaming yourself for slow early progress.

Diastasis Recti: The Hidden Cause of the Mommy Pooch
Diastasis recti is the separation of the rectus abdominis muscles at the midline. As the uterus grows, the connective tissue called the linea alba stretches and thins, creating a gap between the two halves of your abdominal muscle.
A 2025 network meta-analysis published in Scientific Reports found that diastasis recti affects approximately 70% of women in the late third trimester, 60% at six weeks postpartum, and around 30% at one year. That means roughly one in three women still has measurable separation at twelve months, often without knowing it.
When this gap exists, the abdominal wall cannot generate proper tension. Everything pushes outward through the weakened midline, creating that stubborn postpartum belly overhang that does not respond to exercise and does not feel like fat when you press on it.
How to check yourself at home:
- Lie on your back, knees bent.
- Place fingertips horizontally across your midline, just above your belly button.
- Slowly lift your head as if beginning a crunch.
- Feel for a gap or soft, mushy area where your muscles should meet.
- If you can fit more than two fingers in the gap, diastasis recti is likely.
Critical: Traditional crunches, sit-ups, and leg raises worsen diastasis recti. They dramatically increase intra-abdominal pressure directly through the weakened midline. The Cleveland Clinic recommends working with a pelvic floor physical therapist as the gold standard. Even four to six sessions can make a significant difference.
Sleep, Cortisol, and Your Waistline
This is not soft science. A study published in the American Journal of Epidemiology found that postpartum women sleeping fewer than five hours per night at six months had three times higher odds of retaining significant pregnancy weight compared to those sleeping seven or more hours.
The mechanism involves three hormones at once:
- Cortisol rises, directing fat storage toward the abdomen.
- Ghrelin rises, making you significantly hungrier with a drive toward high-calorie foods.
- Leptin drops, reducing your sense of fullness.
Research from the NIH has confirmed that even partial sleep restriction produces clinically significant increases in appetite-stimulating hormones within just two days, underscoring why this is a metabolic issue, not a willpower one.
The result is a hormonal environment designed to stall fat loss, through no fault of your own.
You cannot optimize sleep like a workout schedule since newborns do not cooperate. But you can be deliberate about protecting whatever sleep is available: going to bed when your baby goes down, splitting night duties with a partner, treating naps as a genuine health intervention rather than a luxury.
Chronic stress compounds this. Practical moves that actually reduce cortisol: ten minutes of outdoor walking, saying no to nonessential obligations, calling someone who makes you feel seen. You cannot out-exercise chronic stress, and managing it is part of postpartum recovery.

Safe Exercise Timeline
Always get clearance from your healthcare provider before resuming exercise. ACOG’s clinical guidelines on postpartum exercise note that the six-week mark is a general guideline, not a promise that your body is ready, and that return to activity should be individualized.
| Timeframe | What’s Safe | What to Avoid |
|---|---|---|
| Week 1-2 | Short gentle walks, diaphragmatic breathing, pelvic floor activation | Any exercise beyond slow walking |
| Week 3-5 | Walking 20-30 min, gentle stretching, pelvic tilts | Running, jumping, lifting, crunches |
| 6 Weeks (post-clearance) | Bodyweight squats, modified planks, resistance bands, longer walks | Heavy lifting, high-impact cardio, crunches if diastasis present |
| Month 3-4 | Light strength training, 45+ min walks, low-impact cardio | Heavy barbell work, aggressive calorie restriction |
| Month 6+ | Progressive strength training, moderate cardio, full programs | Anything causing pain, pelvic pressure, or leaking |
| C-Section | Surgeon’s specific guidance; longer recovery before core work | Any movement causing incision pain or pulling |
Walking: Still the Best Starting Point
Walking gets dismissed as “not real exercise.” For postpartum women, especially in the first three months, it is one of the most effective tools available.
A study found that postpartum women accumulating 150 or more minutes of walking per week lost significantly more weight and showed better metabolic health markers than sedentary women. The benefits held even in shorter sessions spread throughout the day.
Walking burns 200-300 calories per hour depending on pace and body weight. It is safe within days of a vaginal delivery (one to two weeks after C-section with physician approval), requires no equipment, and has well-documented benefits for postpartum anxiety, which connects directly to cortisol and fat loss.
Start with 10-15 minutes daily. Add five minutes per week. Work toward 30-45 minutes most days by the end of the first month. Baby in the stroller, baby in the carrier, it does not need to be scenic. It just needs to happen consistently.

Strength Training After Baby
Once you have medical clearance, strength training becomes one of the most effective long-term tools for postpartum belly fat loss. Cardio primarily burns calories during the workout itself, while resistance training helps preserve and build lean muscle mass, supporting metabolic health and improving body composition over time.
A Cochrane review examining diet and exercise interventions after childbirth found that combining physical activity with healthy dietary strategies improved postpartum weight loss outcomes more effectively than no intervention alone.
You do not need a gym to begin rebuilding strength postpartum. These beginner-friendly exercises work well during early recovery:
- Squats: Start with bodyweight only; your baby naturally adds resistance as you progress.
- Glute bridges: Helps reconnect the posterior chain with minimal abdominal strain.
- Wall push-ups progressing to floor push-ups: Builds upper-body and core stability gradually.
- Resistance band rows: Useful for improving posture strain from nursing and carrying.
- Dead bugs: A core-control exercise often tolerated well with diastasis recti.
- Bird dogs: Supports spinal stability without excessive abdominal pressure.
Aim for 2–3 sessions per week lasting 20–30 minutes each. If you notice visible doming or “coning” along the midline of your abdomen during any movement, stop the exercise and consider consulting a pelvic floor physical therapist.
Postpartum Nutrition and Protein
There is no magic postpartum diet. What works is eating enough of the right things. Not restricting, not eliminating food groups, not crash dieting.
The practical framework:
- Fill half your plate with vegetables. High volume, low calories, essential micronutrients.
- Center each meal around protein. Aim for 25-30g per meal.
- Include healthy fats. Avocado, olive oil, nuts, and fatty fish support hormones and lasting satiety.
- Choose complex carbohydrates. Oats, sweet potatoes, quinoa, and legumes provide steady energy and help regulate cortisol. Do not cut carbs postpartum; your brain and body need them.
Research published in Nutrition Reviews found that higher protein intake during the postpartum period was associated with better lean mass preservation and improved body composition outcomes, without compromising milk supply in nursing mothers.
Calorie targets:
| Situation | Minimum Daily Calories | Notes |
|---|---|---|
| Breastfeeding | 1,800-2,200 calories | Below 1,800 risks reducing milk quality and quantity (Academy of Nutrition and Dietetics) |
| Not breastfeeding | 1,500-1,800 calories | A 300-500 cal/day deficit is appropriate |
| First 6 weeks (all mothers) | Eat to recovery | Do not restrict during initial healing |
Protein sources to keep stocked:
| Food | Serving | Protein |
|---|---|---|
| Chicken breast | 4 oz cooked | 35g |
| Cottage cheese | 1 cup | 25g |
| Canned tuna | 1 can (5 oz) | 25g |
| Salmon | 4 oz cooked | 28g |
| Greek yogurt (plain) | 1 cup | 17-20g |
| Eggs | 3 large | 18g |
| Lentils | 1 cup cooked | 18g |
| Black beans | 1 cup cooked | 15g |
Meal prep when possible. Cook double at dinner. Keep fast protein snacks (hard-boiled eggs, cheese sticks, Greek yogurt) within reach. When you are running on empty at 2 p.m. with a baby on your hip, the food that is fastest is the food you will actually eat.
Hydration matters too. Target 8-10 cups of water daily. Nursing mothers need 13 or more cups per day to maintain adequate milk production and support metabolic function. Dehydration is frequently mistaken for hunger. Keep a large water bottle visible, and drink a full glass before each nursing session.
Realistic Fat Loss Timeline
| Timeframe | What’s Happening | Realistic Expectations |
|---|---|---|
| Weeks 1-6 | Uterine involution, hormonal shift, healing | 5-10 lbs from uterus, fluid, blood volume. Not fat loss yet. |
| Month 2-3 | Exercise resumes, metabolism stabilizing | 1-4 lbs of actual fat loss with consistent effort |
| Month 3-6 | Strength building, walking consistent, core healing | 4-8 lbs fat loss, visible belly improvement |
| Month 6-12 | Hormones more favorable, muscle building | 10-15 lbs total lost, significant visible change |
| Month 12-24 | Continued improvement, especially post-weaning | Further fat loss and skin tightening possible |
These estimates assume consistent, non-extreme effort. Results vary based on genetics, starting weight, nursing status, sleep quality, and hormonal response. If you are doing the right things and seeing slower progress, you are not failing. You are healing on your own timeline.
Common Mistakes That Stall Progress
Starting intense exercise too early. Loading a healing pelvis and separated abdominal wall with high-intensity exercise before six weeks can cause real injury and set recovery back by months.
Doing ab exercises to target the belly. Spot reduction does not exist; this has been demonstrated consistently in controlled research.You cannot direct fat loss to a specific area. Traditional crunches with diastasis recti worsen the postpartum pooch. Full-body movement and a modest calorie deficit are what shift fat.
Eating too little. Aggressive calorie restriction increases cortisol, reduces energy for exercise, risks milk supply, and triggers hunger-binge cycles. Eat enough to support your body.
Comparing your timeline to other mothers. Social media surfaces the fastest recoveries. The woman who snapped back in six weeks has different genetics, circumstances, and hormonal response. Her results are not a benchmark.
Depending on compression garments instead of building strength. Waist trainers and wraps compress temporarily. They do not burn fat, improve muscle function, or help diastasis recti. They are a cover-up, not a solution.
Quitting before the six-month mark. Most meaningful belly change happens between months 3 and 12. Stopping at two months (before the timeline even begins) is the most common reason women feel like nothing works.
Myths vs. Facts
| Myth | Reality |
|---|---|
| “You should be back to your pre-pregnancy weight by 6 weeks.” | Your 6-week checkup clears you for activity. It is not a weight loss deadline. Most women need 6-12 months. |
| “Breastfeeding melts the belly fat off.” | It burns extra calories, but nursing hormones often preserve belly fat. Results vary widely. |
| “Waist trainers and belly wraps burn fat.” | They compress temporarily. Fat returns when you remove them. No fat tissue is affected. |
| “Daily crunches are the best way to flatten your stomach.” | Spot reduction does not work. Crunches with diastasis recti worsen the gap. Full-body training is more effective. |
| “You cannot get a flat belly after multiple pregnancies.” | It takes more time and focused core rehab, but many mothers of 2, 3, or more children see significant improvements. |
| “If it has not changed by 12 months, it never will.” | Some women continue improving well into the second year, especially post-weaning. The process is not over at 12 months. |
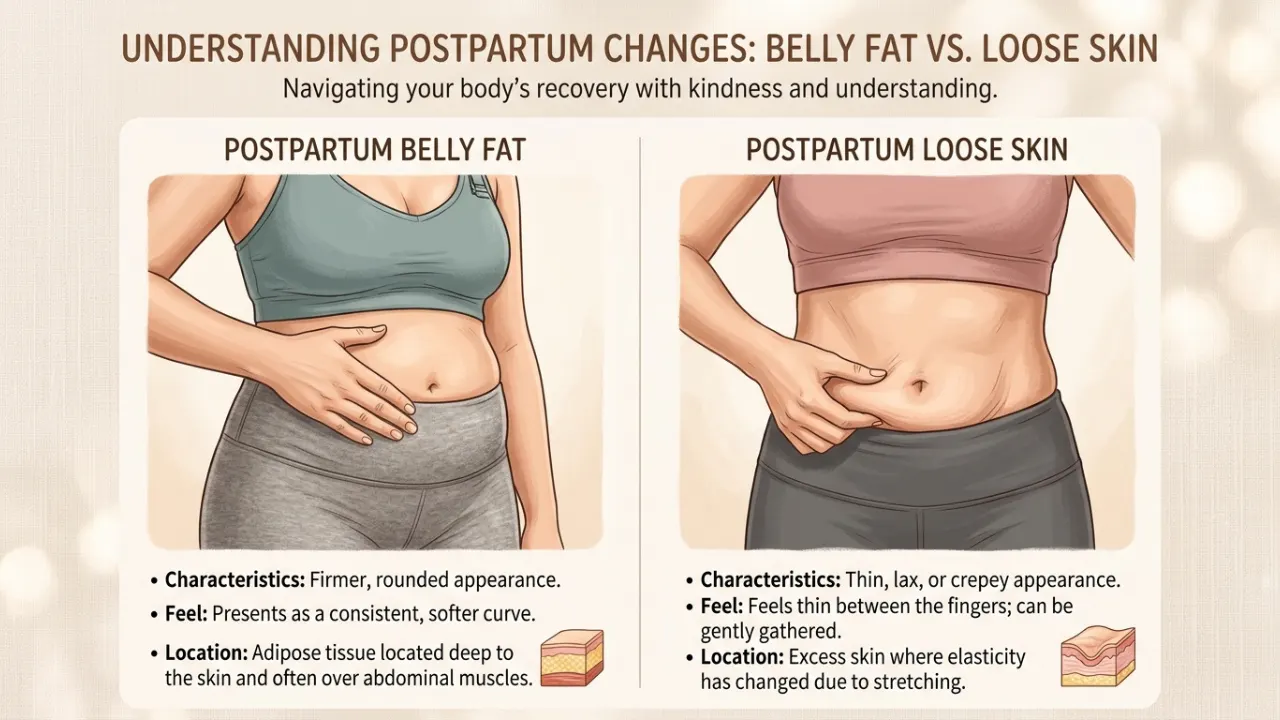
Loose Skin vs. Belly Fat: How to Tell the Difference
These look similar from the outside but respond to different things. Belly fat feels firm under pressure and has a rounded appearance. Loose skin feels thin, almost empty when you pinch it, with minimal fat tissue underneath.
Most postpartum women have some of both, especially in the lower belly below the navel.
Skin elasticity can continue improving for one to two years with hydration, adequate protein (which supports collagen production), and strength training that builds muscle to fill out the area underneath. Genetics, age, and the degree of stretching during pregnancy all play a role.
Loose skin that has not changed after 18 to 24 months of consistent effort may not shift significantly without cosmetic intervention. That is a legitimate medical reality, not a personal failure, and worth knowing.
C-Section Recovery and the Belly Shelf
C-section recovery is abdominal surgery recovery. Multiple tissue layers were cut, and internal healing takes considerably longer than the external scar suggests.
According to the Cleveland Clinic, most surgeons recommend waiting 8-12 weeks before beginning any exercises that significantly engage the deep abdominals, and even then, starting gently with pelvic floor physical therapy guidance.
The “shelf” or overhang that sometimes forms above the C-section scar is a combination of scar tissue adhesion, fat redistribution, and sometimes lymphatic swelling. It can improve over time; scar tissue massage techniques (taught by a physical therapist) can help with the adhesion component. However, it may not resolve completely without cosmetic procedures.
If you had a C-section and are comparing your recovery timeline to vaginal delivery, you are working with a different starting point. Give yourself the extra time your surgery requires.
Mental Health and Body Image
Your relationship with your postpartum body is complicated, and pretending otherwise helps no one. Your body changed dramatically. You may not recognize it. You may feel frustrated, disconnected, or quietly grieving a version of yourself that felt more familiar. Those feelings are real and widely shared.
Postpartum depression and postpartum anxiety affect approximately 15-20% of new mothers, according to research cited by the National Institute of Mental Health, and body image distress is closely tied to both. Obsessive focus on weight loss, constant self-criticism, or exercise and eating behaviors that feel compulsive or punishing can be symptoms as much as they are responses to appearance concerns.
If body image thoughts are taking significant mental energy, or if movement feels like punishment rather than care, please bring this up with your healthcare provider. It is treatable, common, and not something to push through alone.
When to See a Doctor
Contact your healthcare provider if you experience:
- Persistent pelvic, hip, or lower back pain during or after movement
- Urinary or fecal leaking during exercise
- A feeling of pressure or heaviness in the vaginal area
- Visible midline doming during any abdominal exercise
- Your belly appears to be growing after three to four months postpartum
- Still looking significantly pregnant at five to six months with no visible change
- Extreme fatigue that does not respond to rest
- Mood symptoms that feel beyond ordinary new-parent exhaustion
These are not signs your body is broken. They are signals you need professional support to continue safely.
The Bottom Line On How to Get Rid of Postpartum Belly Fat
Your postpartum belly is not a discipline problem. It is not a lack of motivation. It is a biological situation with overlapping causes, and a real, evidence-based path toward resolution.
Walk daily. Add strength training after clearance. Eat enough protein. Protect whatever sleep you can get. Address diastasis recti before doing any traditional ab work. Give yourself the realistic timeline of 6 to 12 months.
These things work. Not dramatically or quickly, but steadily, meaningfully, and sustainably.
The body that grew and delivered a human being deserves patience and care, not punishment. Progress is happening even when it is not visible yet.
Frequently Asked Questions
For informational and educational purposes only. All content on BellyZero, including articles, calculators, health tools, templates, and recipes, is intended to provide general health information. It does not constitute medical advice, a clinical diagnosis, or a substitute for professional healthcare guidance.
Results generated by BellyZero calculators and tools are estimates based on population-level formulas and standard reference ranges. They do not account for your full medical history, individual physiology, existing health conditions, or medications. Results may not apply to pregnant women, children, competitive athletes, or individuals with chronic illness.
Always consult a qualified healthcare professional before making changes to your diet, exercise routine, or health regimen based on anything found on this website. If you have symptoms or concerns about your health, seek medical attention promptly. BellyZero does not accept liability for decisions made based on content published on this site.
Written By: Vikas Arora Updated: May 2026
